Editor’s Note: This video is part of the ongoing allergy series in partnership with Columbia Allergy. To learn more about allergies, eczema, and related topics, please refer to our Allergy Guide!

We found out our son had a food allergy when he was just 6 months old. As parents who do not suffer from food allergies, we were dumbfounded when the first reaction happened. The first reaction was a major one, one that took a 911 call and left us in a state of shock and panic for weeks. We never expected our children to have food allergies – the thought never crossed our minds. On a list of things to worry about and to look out for in babies – SIDS, physical and mental development, soft spots on adorable little heads, latching for breastfeeding, colic, constipation, finances, sleep, household hazards,… so on and so forth – we missed putting “severe allergic reaction” on the list.
If you have any inkling or suspicion that your child may be developing or have food allergies, we’ve compiled – with the help from allergist and immunologist Dr. Jain from Columbia Allergy – some signs to look out for. If you’ve noticed one or more of these symptoms, it may be worth marking down what your child has ingested (and stop feeding those things immediately) and seeking medical advice from your pediatrician or an allergist.
Common Food Allergy Symptoms to Look Out For
Common food allergy symptoms in children can include:
-
Hives
-
Swelling
-
Vomiting
-
Diarrhea
-
Abdominal pain and cramping
-
Fussiness
-
Anaphylaxis
If your child is experiencing any potential food allergy symptoms, it is important to identify the cause so that the food can be avoided or the allergy can be treated to prevent an additional reaction of worsening or life-threatening severity. Allergy testing can be helpful to identify the source of a variety of symptoms.
How do I find out if my child has an allergy?
The best and most accurate way to diagnose an allergy is to make an appointment with an allergist. To diagnose an allergy, the allergist will obtain a detailed history regarding previous reaction details, what caused the reaction, what the symptoms were, how often the reaction has occurred, current diagnoses, and medications. In addition to the history, the provider will recommend allergy testing to determine the source of the allergic reaction and the severity of the allergy.
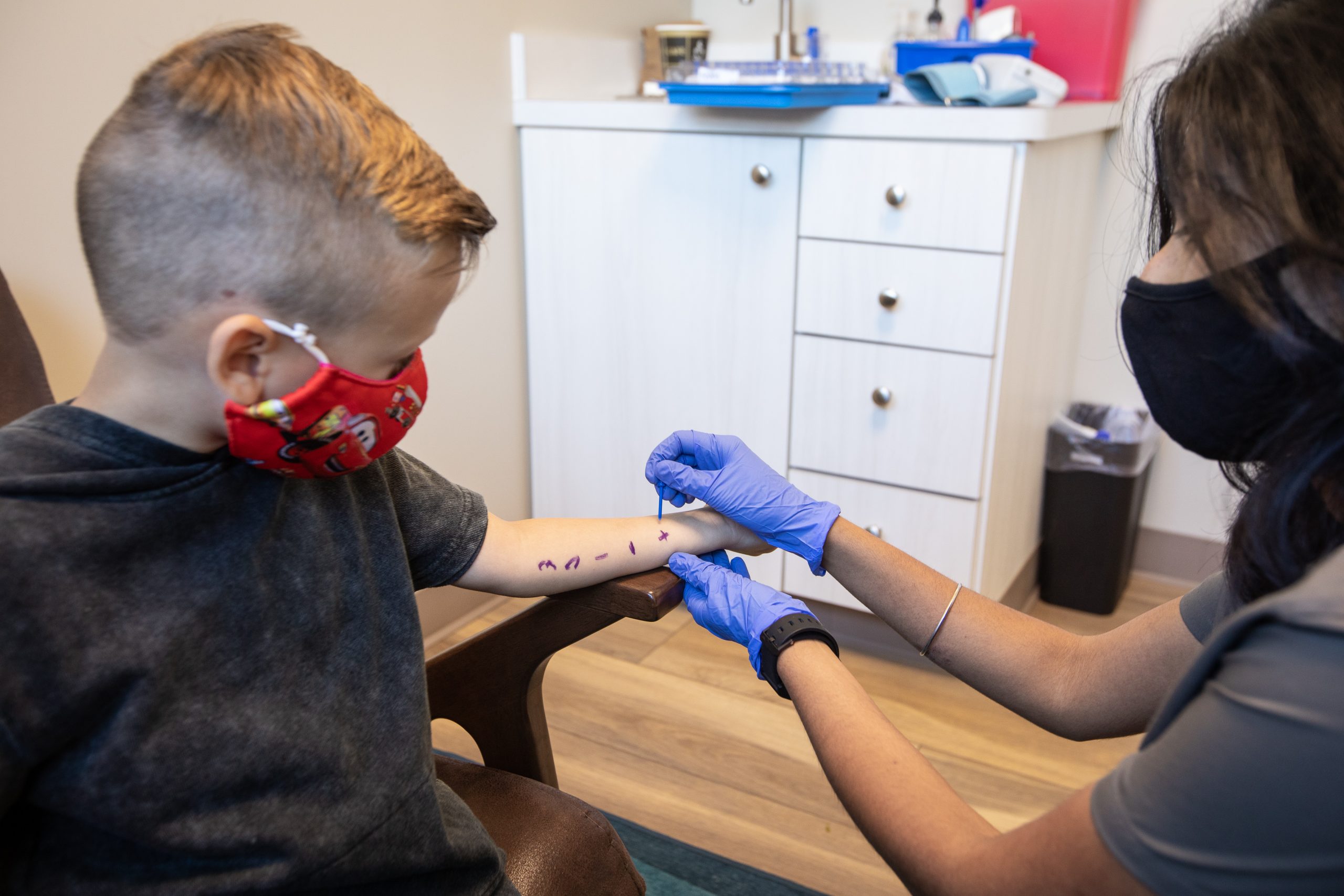
Skin prick testing can be useful in identifying potential food allergies. This test uses a pointed plastic device to apply potential allergens in a liquid form to the skin, usually on the back. After the allergens are applied, the patient will wait for 20 minutes to see if a reaction occurs to the allergens applied to the patient’s skin. In addition to determining which foods cause a reaction, this test can also help to identify the severity of these allergies based on the size of the reaction. If an allergy is present, the patient may develop an itchy, red bump at the location of the prick site on their skin. The itching will often resolve in several hours and can be managed with an antihistamine or topical medication if uncomfortable.
No allergy test is 100% accurate, but when used in coordination with a patient’s history skin prick testing is well-recognized as an appropriate method for testing for IgE mediated food and environmental allergies. Skin prick testing is a common allergy testing method since it offers immediate test results and may be less traumatic than a blood draw for some children. For an allergy test with blood, a patient’s blood will be drawn at a lab. The blood will then be tested to see if antigen-specific antibodies (IgE) exist, and how many antibodies exist for the specified antigens. If antigen-specific antibodies exist, it means that the patient’s body has identified this substance as foreign and has created antibodies to protect the body from this specific substance. If an allergen has high numbers of IgE that are present, this typically indicates a more severe allergy.
The information on this website is not intended or implied to be a substitute for professional medical advice, diagnosis, or treatment. All content, including text, graphics, images, and information, contained on or available through this website is for general information purposes only. Always seek the advice of your physician or other qualified health care provider with any questions you may have regarding a medical condition or treatment and before undertaking a new health care regimen. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.